By Bigboy Madzivanzira
Introduction
As the rain season intensifies, snake encounters are surging across Zimbabwe. Recent Ministry of Health reports show 147 snakebite cases and 2 deaths in a single week (Bindura and Chegutu) , 167 bites with no deaths in another week, and a cumulative total of 3,018 cases and 10 deaths for 2025. Earlier figures show 1,686 cases and 6 deaths by early April 2025. Compared to previous years, the numbers are rising fast. 707 cases and 3 deaths in 2023, 2,917 cases and 14 deaths in 2024. Most bites happen between November and April, when snakes are most active and rural communities are exposed during farming and outdoor activities .
Case Study
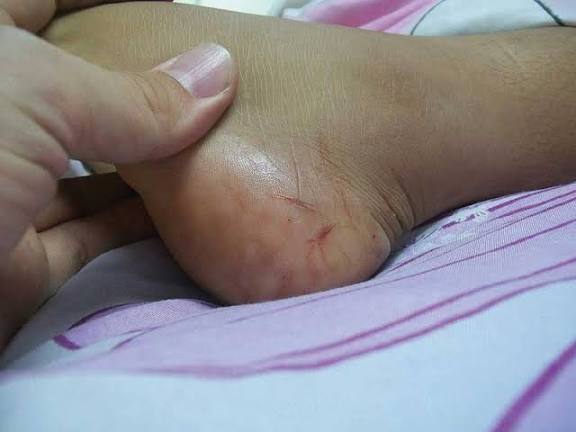
A recent tragedy that highlights this crisis involved a school-going boy bitten by a black mamba while hunting birds. Without immediate antivenom, such cases often end in death or amputation, showing how deadly the gap in emergency care can be.
Regional Perspective
Zimbabwe’s snakebite crisis mirrors a broader regional challenge. Sub-Saharan Africa records between 90,000 to 420,000 snakebite cases annually, with 4,000 to 30,000 deaths. In West Africa, a 16 country study showed that the cost per death averted from snakebites ranges from $1,997 in Guinea-Bissau to $6,205 in Liberia and Sierra Leone, with cost per DALY (Disability-Adjusted Life Year) averted ranging from $83 in Benin to $281 in Sierra Leone. South Africa, home to the only sub-Saharan antivenom producer (South African Vaccine Producers), still faces occasional shortages, forcing reliance on imports from India. East and Central African countries like Kenya, Uganda, Tanzania, and DRC also report under-reported cases and weak antivenom supply chains.
District-Level Breakdown (Zimbabwe)
– Mashonaland Central (Bindura): Recorded 147 cases and 2 deaths in one week (June 2025).
– Mashonaland West (Chegutu): Part of the same spike, with multiple cases reported.
– Midlands Province: Reports show high numbers of cases in rural districts, especially during peak farming season.
– Masvingo and Matabeleland: Though data is limited, anecdotal reports from clinics indicate frequent snakebite cases with delayed treatment due to distance from major hospitals.
Successful Antivenom Distribution Examples
– South Africa: The South African Vaccine Producers (SAVP) supplies antivenom across the country and exports to neighboring nations, reducing mortality where distribution networks are strong.
– Kenya: Pilot programs using mobile health units and regional antivenom stockpiles have improved response times in rural areas, cutting down on deaths.
– India: Though outside Africa, India’s centralized antivenom procurement and state-level distribution hubs have been cited as a model for low and middle-income countries.
Call to Action
This situation calls for urgent action:
– Strengthening supply chains to ensure antivenom reaches remote clinics.
– Training healthcare workers in snake bite management and antivenom administration.
– Exploring collaboration between modern health practitioners and recognized traditional healers to create a bridge of trust and safety for patients.
– Public awareness campaigns on prevention and first aid for snake bites.
As a Health Promotion Practitioner, I believe addressing this issue requires a multi-sectoral approach that respects community knowledge while ensuring access to life-saving medical treatment. No one should lose a limb or life simply because help is too far away.
About the Author
Bigboy Madzivanzira is a journalist and certified Medical Rehabilitation Practitioner passionate about improving healthcare access and rehabilitation services across Zimbabwe. He writes on health systems strengthening, disability inclusion, and workforce development.
📞 Contact: 0773 367 913
✉️ Email: healthpromotionclinic@gmail.com